Are you tired of suffering from the constant discomfort of acid reflux and the effects it has on your quality of life? You’re not alone. Acid blockers are often the first line of defense for those grappling with GERD (gastroesophageal reflux disease), but what if these widely prescribed medications don’t actually work? In this myth-busting journey, we’ll delve into the truth about acid reflux, why acid blockers may not be the solution, and how you can finally conquer your acid reflux for good.
How Acid Reflux Happens: Let’s Break it Down
Stomach Acid is Not The Enemy
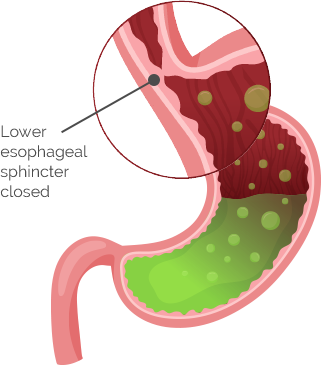 Stomach acid plays a vital role in the functioning of your digestive system. Adequate stomach acid levels signal the LES to tighten, preventing acid from escaping into the esophagus. Factors like aging, stress, caffeine, certain medications (especially proton-pump inhibitors), and alcohol can lead to a condition known as hypochlorhydria, where stomach acid production decreases. With that in mind, you can see how further blocking stomach acid with PPIs could wreak havoc with your system and create even more overall health issues.
Stomach acid plays a vital role in the functioning of your digestive system. Adequate stomach acid levels signal the LES to tighten, preventing acid from escaping into the esophagus. Factors like aging, stress, caffeine, certain medications (especially proton-pump inhibitors), and alcohol can lead to a condition known as hypochlorhydria, where stomach acid production decreases. With that in mind, you can see how further blocking stomach acid with PPIs could wreak havoc with your system and create even more overall health issues.
The Dangers of Acid Blockers
As noted, PPIs are medications that suppress stomach acid production. Where these medications catch people out is they can create a short-term fix situation that gives the person so much relief that they don’t consider the long-term side effects or outcome. The problem is that while PPIs may temporarily alleviate symptoms, they fail to address the root issue, the malfunctioning LES.
 Nearly 20 percent of adults regularly use acid-lowering drugs like proton pump inhibitors. However, as many as 70 percent of people experience no benefit from taking them, and they may even worsen the underlying condition: low stomach acid. This highlights a critical flaw in the approach of using antacid medications to address acid reflux.
Nearly 20 percent of adults regularly use acid-lowering drugs like proton pump inhibitors. However, as many as 70 percent of people experience no benefit from taking them, and they may even worsen the underlying condition: low stomach acid. This highlights a critical flaw in the approach of using antacid medications to address acid reflux.
Gastroenterologist Dr. Kyle Staller warns against long-term PPI use, stating that many individuals derive no benefit and continue taking them unnecessarily. Worse yet, studies associate PPIs with vitamin B12 deficiency, reduced calcium absorption, increased pneumonia risk, hip fractures, heart attacks, chronic kidney disease, dementia, and even stomach cancer. Discontinuing PPIs often leads to rebound acid reflux symptoms which can be very tough to experience. This is something we help our clients through when transitioning off PPIs with our Heartburn Relief Kit which works on rebuilding the stomach acid whilst soothing and reducing inflammation in the stomach and esophagus.
Why AND When Do Stomach Acid Levels Drop?
You likely don’t recall having heartburn or acid reflux that often when you were younger and that’s because stomach acid is something that tends to decline with age. In one study on this topic, researchers found that acid production was reduced by about 30 percent in men and women 65 and older. So given that stomach acid generally decreases with age but the prevalence of heartburn symptoms goes up, it makes sense that low stomach acid is causing acid reflux rather than an excess.
There are other factors that can reduce stomach acid that you can work on improving to ease your symptoms, so these should definitely be noted. Such factors include:
- Stress: Chronic stress can lead to imbalances in the digestive system, affecting the production of stomach acid.
- Medications: Certain medications, such as proton-pump inhibitors (PPIs), antacids, and H2 blockers, can suppress stomach acid production.
- Diet: A diet high in processed foods, refined sugars, and low in nutrient-dense foods can affect stomach acid production. Excessive alcohol consumption and caffeine intake may also contribute to low stomach acid levels.
- Chronic Infections: Infections like H. pylori can interfere with stomach acid production and lead to digestive issues.
- Digestive Disorders: Conditions such as gastritis, celiac disease, Crohn’s disease, and atrophic gastritis can damage the stomach lining and impair acid production.
- Autoimmune Conditions: Some autoimmune disorders can target the cells in the stomach lining responsible for producing stomach acid, leading to reduced acid levels.
- Nutrient Deficiencies: Low stomach acid can hinder the absorption of essential nutrients, such as vitamin B12, iron, and calcium, leading to deficiencies that may exacerbate the issue.
- Lifestyle Factors: Eating too quickly, not chewing food thoroughly, or consuming large meals can strain the digestive system and impact stomach acid levels.
- Smoking: Smoking can weaken the lower esophageal sphincter (LES), causing bouts of reflux.
Now You Have the Intel, It’s Time to Take Action!
 If you take anything from this article, let it be this: suffering from acid reflux doesn’t mean you’re doomed to a lifetime of discomfort and acid blockers. Now that you understand the true nature of acid reflux, you can build up your stomach acid with supplements like the HCL in our Reflux Inhibitor and adopt a more holistic approach to your digestive health. Within a few months, your acid reflux will be a thing of the past and you’ll be much more in tune with your body as a whole.
If you take anything from this article, let it be this: suffering from acid reflux doesn’t mean you’re doomed to a lifetime of discomfort and acid blockers. Now that you understand the true nature of acid reflux, you can build up your stomach acid with supplements like the HCL in our Reflux Inhibitor and adopt a more holistic approach to your digestive health. Within a few months, your acid reflux will be a thing of the past and you’ll be much more in tune with your body as a whole.



